
Anaphylaxis and Severe Allergic Reaction
This Factsheet has been written to provide information on severe allergic reactions which have an immediate or rapid type onset...
 Reducing allergic reactions to food | Allergy UK | National Charity
Reducing allergic reactions to food | Allergy UK | National CharityA parent and carer resource
This leaflet has been created by leading experts in allergy, with the aim to assist parents and carers in reducing the chances of their child experiencing a severe allergic reaction to food. It offers advice, information and tools to help effectively manage their condition with confidence.
This Patient Information Sheet has been written by Dr Nandinee Patel, Dr Ru-Xin Foong, Dr Paul Turner, Prof Graham Robers and Prof Adam Fox. It has been reviewed and endorsed by Allergy UK .
Download the leaflet to empower yourself when caring for your child with a food allergy
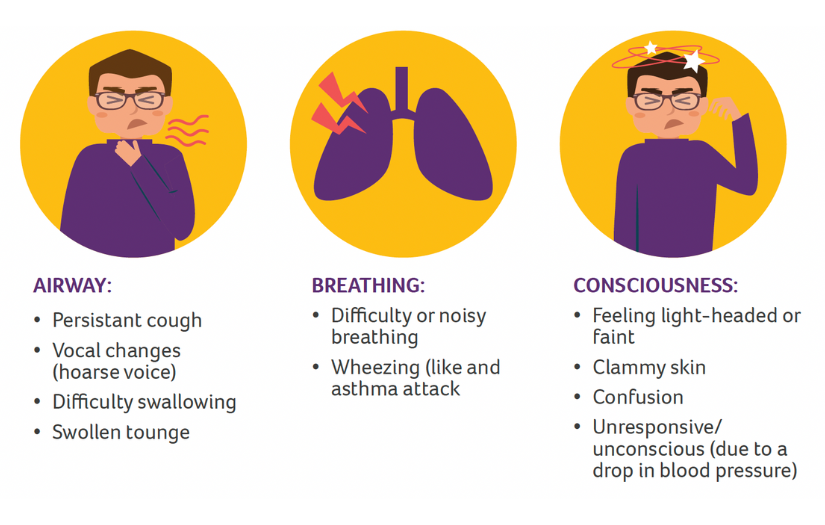
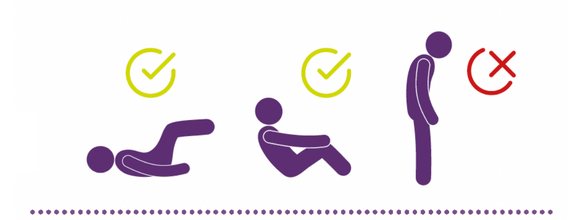
This leaflet explains how you can reduce the risk of this happening. Anaphylaxis is unpredictable and can occur in people who have never had this type of reaction before, but most people will recover fully.

This Factsheet has been written to provide information on severe allergic reactions which have an immediate or rapid type onset...

Anaphylaxis (pronounced ana- fill – axis) is a medical emergency, common causes of anaphylaxis include food, wasp/bee venom (stings) and...

Anaphylaxis is a severe and potentially life-threatening allergic reaction. It usually comes on within minutes of being exposed to the...