
Chronic Spontaneous Urticaria (CSU) Poster
Chronic Spontaneous Urticaria (CSU) is a common and distressing skin condition that causes itchy and sometimes painful hives or wheals...
 Chronic Spontaneous Urticaria Leaflet | Allergy UK | National Charity
Chronic Spontaneous Urticaria Leaflet | Allergy UK | National CharityChronic Spontaneous Urticaria (CSU) is a common and distressing skin condition that causes itchy and sometimes painful hives or wheals (raised rash or patches) on the skin with no known obvious cause or trigger.
The rash can be tiny bumps or large raised patches of different shapes and sizes and can affect any part of the body. Sometimes the rash can be accompanied by swelling called angioedema.
To be classed as chronic, the wheals (urticaria) must be present daily for at least six weeks.
It is called ‘spontaneous’ when you cannot identify a reason for the symptoms to appear.
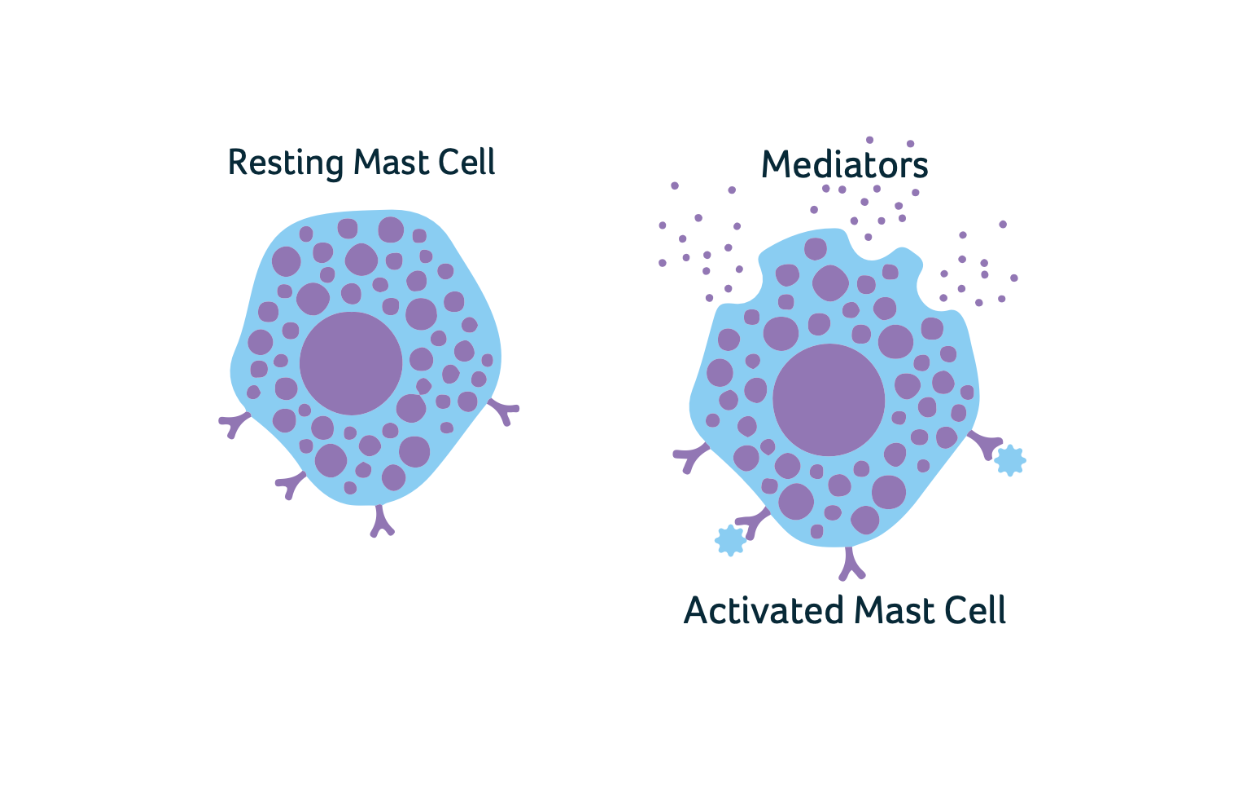
In our immune system we all have mast cells, which are cells that circulate in the blood and are found in most tissues in the body.
Mast cells help the immune system to reduce inflammation, fight infection and assist with wound healing and repair. When you experience urticaria, mast cells in
the immune system are activated due to
a signal (trigger) and release chemicals, including histamine, into the skins tissue, causing the red itchy raised rash, often referred to as hives.
Research suggests that in about 50% of people with CSU, the cause of their CSU is autoimmune. This is when the body mistakes its own cells as harmful and so activates cells including mast cells which then cause the symptoms of urticaria.
CSU is a visible skin condition that can be painful, with flare ups being very unpredictable and affecting your ability to do your usual activities. CSU can affect:
NO. CSU is not caused by allergens (substances which cause an allergic response) or an allergic reaction. Allergy testing, elimination diets, and avoidance of the usual triggers are not always useful in trying work out the cause or manage symptoms. It is true that for some people, there may be things that can make their CSU worse, but they won’t cause CSU. This is what makes CSU different from other urticarial skin reactions is that there is often no known trigger or cause.
Soothe the skin:
Try to avoid scratching – Scratching releases more itch chemicals (histamine) and will make you itch more.
Wearing loose light clothing – This helps to reduce itch and make you feel more comfortable.
Try to relax – Reduce stress and avoid stimulants – In some people avoiding alcohol, recreational drugs, caffeine or extremes of temperature can help reduce symptoms.
Avoiding certain medications – Aspirin, non-steroidal anti- inflammatory (NSAIDS), opiates e.g., codeine and ACE inhibitors can make the symptoms of CSU worse in some individuals. If youare on these medications, speak to your doctor about stopping them before you do.
If you suspect you have CSU you need to speak to your from your GP or other healthcare professional. Your health care professional may carry out diagnostic testing to make sure your symptoms are notcaused by any other medical conditions. They may also ask you to keep a symptoms diary or complete a CSU severity scoring system to help them to assess how severe your symptoms are.
To be diagnosed with CSU your symptoms need to be present daily for at least six weeks, and it may take a few appointments with your GP or healthcare professional to get diagnosed with CSU.
Taking a daily nonsedating antihistamine. For most people, this will stop the symptoms. Medical guidelines recommend that doctors can increase antihistamines up to four times the normal daily dose to achieve symptom control.
If antihistamines are not effective, then a tablet called a Leukotriene receptor agonist can be tried to see if this helps reduce your symptoms. Sometimes a one-off short course of corticosteroids tablets may also be offered for severe flare ups.
The next step is to try immunosuppressive treatments, such as ciclosporin. This treatment is designed to supress the immune system and is usually started by a specialist in hospital, as it requires regular blood test monitoring to reduce the risk of side effects.
Where other treatments haven’t helped, newer treatments called biologic therapies can be given. Biologic therapies are used to target a certain part of the immune system and switch off or block the immune cells that are causing the symptoms. These treatments are only available from specialist hospital departments.
It is important to ask for help if:
If you feel your symptoms are not being managed well enough, speak to your healthcare professional. They can refer you for specialist treatment if it is necessary. Do not suffer in silence, help is available for CSU.

Chronic Spontaneous Urticaria (CSU) is a common and distressing skin condition that causes itchy and sometimes painful hives or wheals...

Chronic Spontaneous Urticaria (CSU) is a common and distressing skin condition that causes red, raised, itchy and sometimes painful wheals...

What is Chronic Spontaneous Urticaria (CSU)? Chronic Spontaneous Urticaria (CSU) is a common and distressing skin condition that causes red,...
This leaflet has been produced with the support of Novartis.