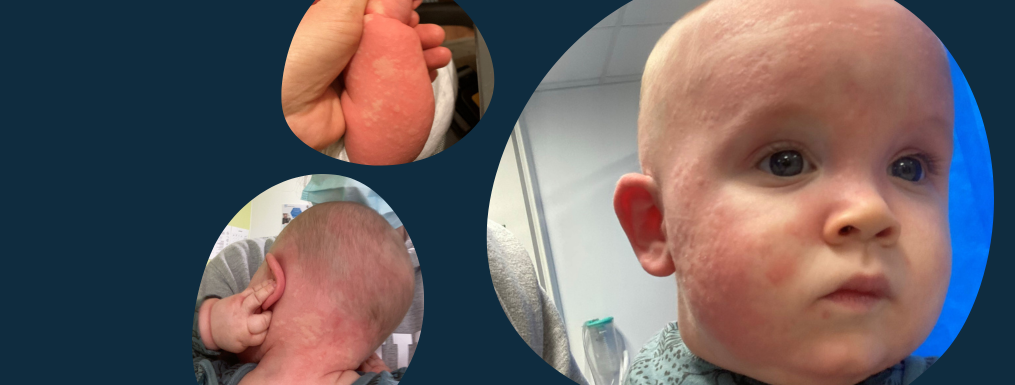
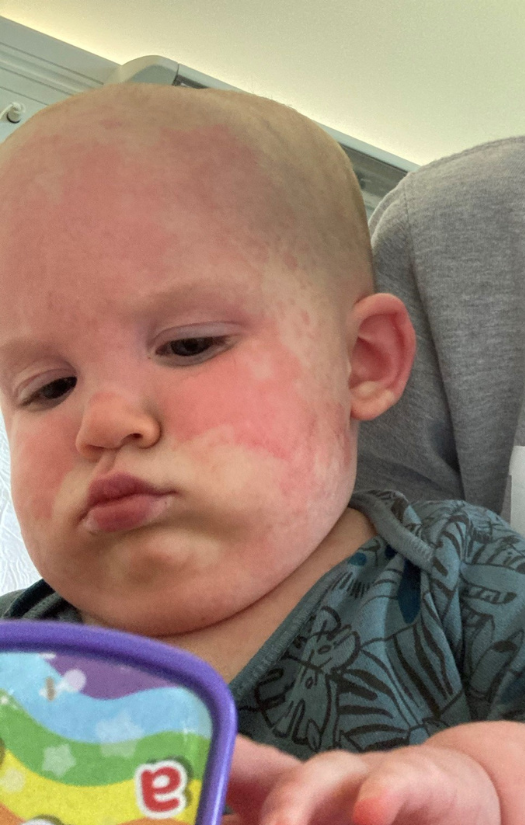
Max always had terrible skin from the moment he was born. Within a couple of months, his skin was just dry often under his neck and the top of his chest. Naively, I thought he was just dribbling so I put a bit of mild baby cream on it which did nothing. It was then I had to see a GP and sent pictures via an eConsult which resulted in them prescribing topical steroids. After a couple of weeks off the steroids, his dry skin would reappear. I received no guidance on how eczema could be linked to anything that I was feeding him. Management was kept very separate, treating eczema with steroid and food allergy with elimination.
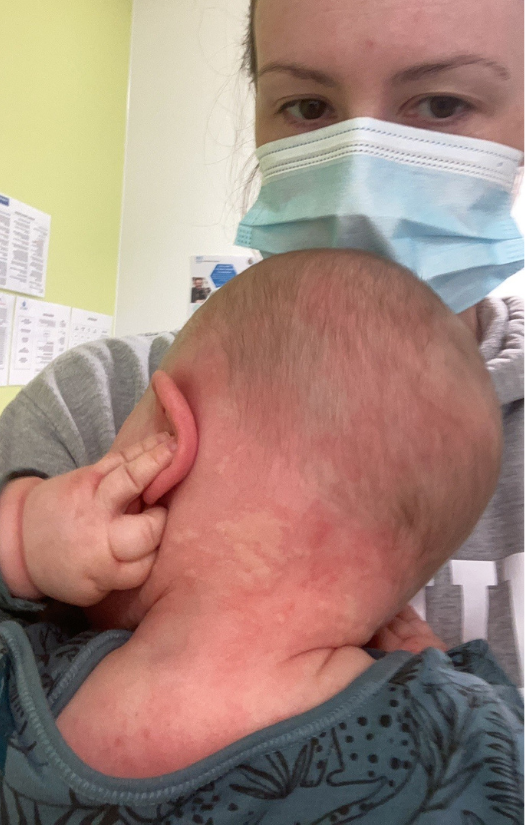
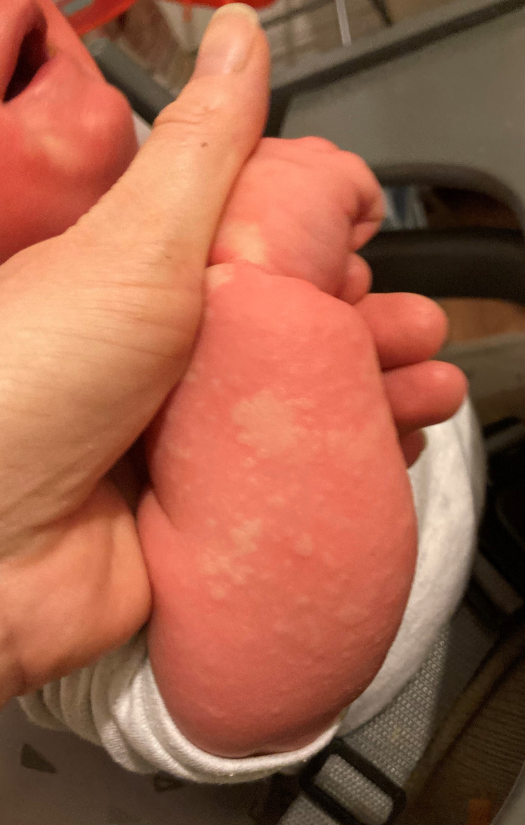
At 10 months, Max had a reaction to peanuts. I’d been feeding him almond butter for breakfast, and that morning I just picked up the peanut butter. Not thinking anything of it. He started to cough and get hives on his face. I had seen this before. Within minutes, he was covered in widespread hives all over his body. Max’s previous reaction to milk meant I recognised the hives as a symptom of an allergic reaction. Although, at the time, I didn’t know the severity of the reaction.
We took him to a hospital with an urgent care centre and were seen quickly by their GPs. He had a secondary reaction whilst with the GP. The welts on his body were huge, it wasn’t just like nettle stings or hives. It was almost like a map. Imagine like a world map all over my child’s body. Max was given a steroid, which he just threw up everywhere. Then I was told, ‘We can’t help you here, you have to go to the hippo ward at a hospital 30mins away. Are you okay getting there by yourself?’
Knowing what I know now, I shouldn’t have been left driving my 10-month-old baby having an allergic reaction whilst navigating 9am traffic. I remember, during the journey looking back at my child, who looked incredibly sad. All parents know when something is wrong with their child – you can see it in their eyes. His look will never leave me. We got to the ward and were monitored for six hours. He was given another steroid. They never mentioned anaphylaxis but did refer us to an allergy clinic.
I still hadn’t had my referral appointment – it was verging on a nine to 12 months wait by that time. The private consultant mentioned anaphylaxis, having no idea what that meant. He prescribed AAIs (EpiPens) and explained how to use them. He did skin prick tests and blood tests. We’d previously had blood tests for the cow’s milk allergy, which included peanuts, which was negative, but he hadn’t been exposed really to peanuts at that time.
After I started reading Facebook groups of parents with children with allergies and realised what it meant for my child, moving forwards. A lot of personal traumas occurred after the event. It was traumatic, having witnessed my child in that situation. But it was even more traumatic to have to connect the dots myself and make sense of the situation. It’s not right that the NHS didn’t tell me that he that he’d suffered anaphylaxis and didn’t issue the lifesaving medication he needed.
Most information I’ve received has been from other allergy families, people who have been in this situation, people who have access to specialist allergy care that we don’t necessarily have in our area. Telling us what questions to ask and how to be advocate from my child in appointments.
The journey starts with the GP as they are the first port of call for all families. GP’s need to be better equipped with knowledge on where to signpost to, specialist referral paths and clear guidance for recognising the signs of anaphylaxis and ringing 999. How many children out there need lifesaving medication and don’t have it?

 Helpline
Helpline