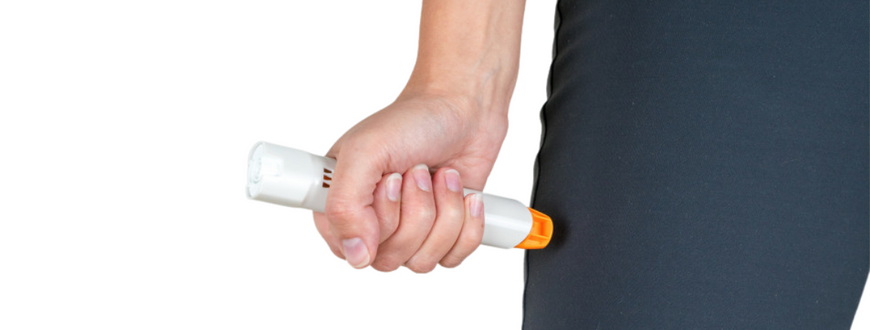
Adrenaline auto-injectors
This information factsheet has been developed to highlight the importance of carrying your adrenaline auto-injectors. It will also cover the different types and brands of adrenaline auto injectors available in the UK as well as how to care for your adrenaline auto injector.

 Helpline
Helpline